Elephantitis (Elephantiasis)
Last reviewed by Dr. Raj MD on January 12th, 2022.
Have you ever seen a person with insanely swollen lower body? There are chances that the person may be suffering from a serious condition called elephantitis. The medical term for this disease is elephantiasis or lymphatic filariasis, however, it is commonly misspelt as elephantitis. Elephantiasis is endemic to the tropical and subtropical regions and it has claimed may lives.
What is Elephantitis?
As the name suggests, elephantitis is a medical condition that causes swelling and thickening of the skin and underlying tissues to a humongous size, mostly on the arms, legs and genitals. In males, elephantiasis is characterized by abnormal inflammation on the skin surrounding the penis, scrotum or testicles. This condition is called as elephantiasis of the penis, testicular elephantiasis or elephantiasis of the scrotum. In females, elephantiasis causes inflammation in the vagina, labia minora or breast. Apart from genitals; head, feet, nose and hands are also very prone to elephantiasis.
What are the Different Types of Elephantiasis?
Accumulation of excessive lymphatic fluid, especially in the lower torso, is called as lymphedema. Elephantiasis develops if the lymphedema is permanent and the lymphatic drainage is irreversibly compromised. Elephantiasis is majorly classified into two types – lymphatic and non- filarial elephantiasis. Other types of elephantiasis include elephantiasis nostras and proteus syndrome.
What Causes Elephantitis?
Lymphatic filariasis
Lymphatic filariasis, also called as filarial elephantiasis, is the most common type of elephantiasis. Lymphatic filariasis is caused due to infection by various parasitic worms. These parasites which cause elephantiasis are transmitted through mosquitoes.
The exact mechanism of the disease occurrence is not yet understood. However, it is believed that the parasites causing lymphatic filariasis grow and multiply within the lymphatic system. The worms secrete some kind of toxins within the lymphatic system that causes the body to generate an immune response. This immune response may be expressed in the form of an allergic reaction that may cause dilation of the lymphatic vessels, medically called as lymphangiectasia. Lymphatic system is made up of many nodes and vessels that run throughout the body. The lymphatic system is responsible for draining out the excess tissue fluids that did not travel into the bloodstream, clearing the debris or microorganisms from the lymphatic fluid and returning the fluid to the bloodstream.
Therefore, any obstruction or damage to the lymphatic system or the lymphatic vessels leads disturbances in the lymphatic drainage. This in turn leads to swelling and inflammation in the body due to accumulation of lymphatic fluid, especially the limbs, genitals and breasts. Sometimes, bacterial infections may occur in the areas affected by elephantiasis which may further worsen the condition.
In some cases, swelling causes due to filarial parasitic infection goes to such an extent that it may become impossible to cover up the affected area.
Non- filarial Elephantiasis
The other type of elephantiasis called as non- filarial elephantiasis is not caused due to parasitic infection. Non- filarial elephantiasis, also known as podoconiosis, occurs due to continuous contact with soil such as red clay and volcanic by- products. Volcanic ash and red clay containing alkali metals such as potassium or sodium may cause irritation to the skin thereby causing inflammation in the exposed areas of the skin. This may lead to the skin turning hard and fibrotic over the time. Non-filarial elephantiasis almost in all the cases occurs only in the feet and leg. Very rare cases of non- filarial elephantiasis above the knee have been reported. A person’s vulnerability to developing allergic reactions to alkali metals or volcanic ash may be decided by genetic factors.
In some cases, diseases such as tuberculosis, leprosy, leishmaniasis or sexually transmitted diseases such as lymphogranuloma venereum may cause permanent damage to the lymphatic system, thereby causing formation of elephantitis. Non- filarial elephantiasis may also be caused due to a medical condition known as edema which leads to accumulation of fluids in the body, thereby causing inflammation and swelling in various parts of the body.
How do you get Elephantitis?
Lymphatic filariasis is caused when elephantiasis parasites or worms damage the lymphatic system of the body, whereas, non-filarial elephantiasis occurs due to a person’s susceptibility to volcanic ash.
The lymphatic filariasis parasites such as Brugia timori, Wuchereria bancrofti, symbiotic Wolbachia bacteria and Brugia malayi enter into the body due to a mosquito bite (mostly due to female Anopheles, Aedes and Culex species of mosquito). When the mosquito bites a human, it transfers the larvae to the lymphatic system via the skin. The larvae grow within the lymphatic system to turn into a full grown parasite. The transformation of larvae to parasite occurs slowly over a period of approximately 7 years (in some cases even 40 years).
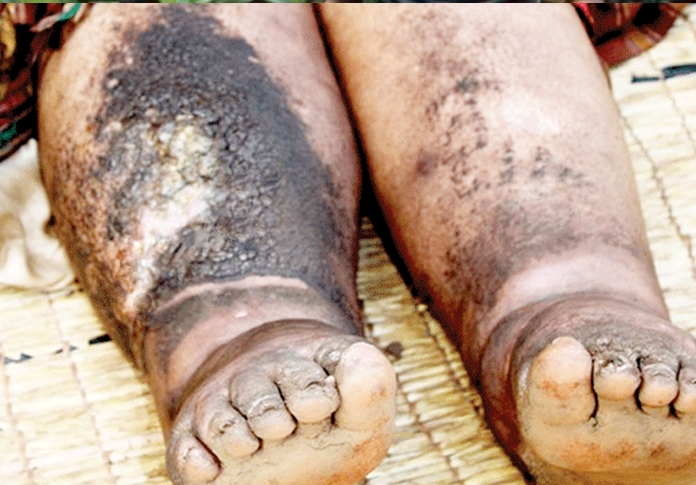
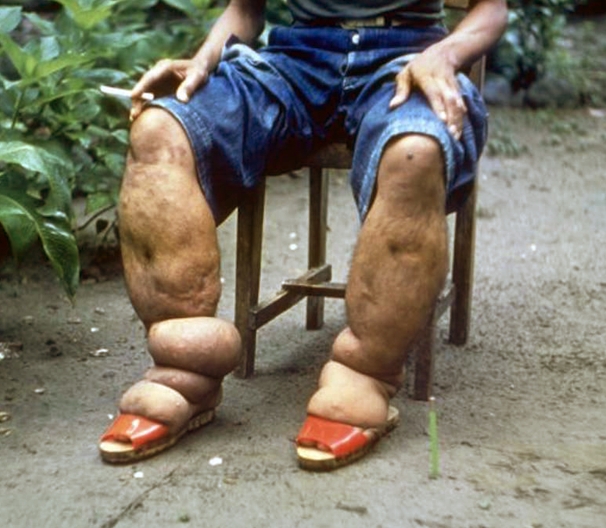
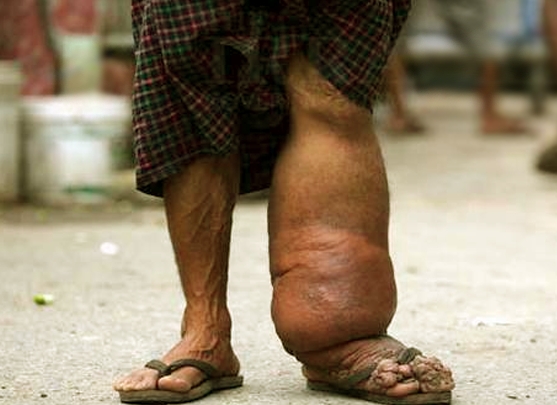
Elephantiasis Pictures
Take a look at these pictures to get a better understanding about what elephantiasis looks like.
What are the Symptoms of Elephantiasis?
Symptoms of elephantiasis are dependent on the cause of the disease and in most cases, the symptoms are presented only at a later stage of the disease.
Filarial elephantiasis – A person with lymphatic filariasis may sometimes show no major symptoms of elephantiasis. Whereas in some cases; acute or chronic symptoms may be seen in a person infected with filarial parasites. As previously mentioned in this article, swelling and thickening of skin and underlying tissues is one of the main signs of elephantiasis. Swelling and inflammation of the skin occurs as a result of swelling in the lymph nodes. Swelling is commonly observed on the lower part of the body, however, head, hands and breast are also prone to get swollen due to elephantiasis.
Inflammation in elephantiasis is accompanied with unbearable pain in the affected area. Fever associated with shivering and perspiration may also be seen in patients suffering from elephantiasis. These symptoms are manifested as a result of the body’s natural tendency to fight the parasite causing elephantiasis. In some cases, rashes, tenderness and hyperpigmentation may also be observed on the affected areas of the skin. Skin ulcers, abscesses and wrinkles may also be observed in some people. Sometimes, bacterial growth occurs in these abscesses and ulcers, thereby causing pus accumulation and tenderness in the affected areas of the skin. In chronic cases, organs such as liver and spleen may also get enlarged.
Elephantiasis of the scrotum and testicle presents signs such as disproportioned growth of the scrotum and testicles, sometimes to enormous size. This not only causes pain and physical disabilities to the patient, but also leads to embarrassment and social outcast. Genital elephantiasis in females may lead to growth of painful tumors in the vagina and labia minora, which may even spread to the vulva.
Most of the symptoms of elephantiasis resemble the symptoms of lymph node related diseases such as lymphedema or hydrocele.
Non- filarial elephantiasis – The early symptoms of non- filarial elephantiasis may include burning and itching sensation in the lower leg, mainly feet. The soles of the feet may become tender and swollen and pus accumulation may be seen. Additionally, pain in the legs, inflammation of the legs and fever may also be presented as symptoms of non- filarial elephantiasis. Eventually, the skin on the affected areas may become thick and hard and may have a warty appearance.
Is Elephantitis Contagious?
Lymphatic filariasis which is caused due to transmission of parasitic worms by mosquitoes is a contagious disease. Lymphatic filariasis is contagious even during the stage when larvae are getting converted into full- grown parasites. The infected person may not even show any symptoms of elephantiasis at this stage. An infected mosquito can however transfer the parasite/ larvae from one person to another. In most cases, the mosquitoes transfer the larvae of the parasite, rather than the full grown parasite itself, into the human host. Though the filarial parasites grow within the lymph nodes, larvae of these parasites have the ability to penetrate into the bloodstream and can obstruct the blood flow through the blood vessels or the nodes. Other serious medical conditions such as gangrene and streptococcal lymphangitis may precipitate as a result of elephantiasis larvae infection.
However, non- filarial elephantiasis is caused due to a person’s vulnerability to alkali metals and volcano ash. This type of elephantiasis is very commonly seen in rural areas, where people often walk barefoot. Travelling barefoot causes the people to get exposed to various alkali metals present in the soil, which may cause obstruction in the lymph node and subsequently may cause elephantiasis. Non- filarial elephantiasis is also common in areas prone to disasters such as volcanic eruptions.
Elephantitis Diagnosis
Accurate diagnosis of the cause of elephantitis is essential for deciding the course of treatment. Elephantiasis presents signs and symptoms very similar to those manifested in other lymphatic system related issues. Therefore, it may be an arduous task to distinguish filarial elephantiasis from non- filarial elephantiasis or lymphatic system related disorders using simple diagnostic methods.
- Blood tests may help in diagnosing the disease and in differentiation between filarial and non- filarial elephantiasis. Complete blood count of a person suffering from filarial elephantiasis may show high levels of eosinophils. Various other blood tests such as ELISA, PCR or finger prick card tests may help in identification of filarial elephantiasis.
- Microscopic tests such as cytology that make use of powerful microscopes to detect the presence of parasites may prove to be a useful method in accurate diagnosis of elephantiasis.
- Ultrasound visualization of the affected areas such a scrotum may help in visualization of the movement of filarial causing parasites.
- Yet another way of diagnosing elephantiasis is by carrying out a biopsy of the lymph node. This method is however not the method of choice for diagnosis of elephantitis.
Can Elephantiasis Be Treated?
Sadly, there is no absolute cure for elephantiasis. Also, no vaccines have been invented yet to prevent elephantiasis from occurring in the first place. Albeit, the good news is that a vaccine to treat elephantiasis may soon be introduced in the market. However, one has to seek medical help in case of elephantiasis to reduce the symptoms of elephantiasis (if possible) and to get some relief from the pain.
Treatment of elephantiasis involves cleaning the affected areas of the skin thoroughly on a regular basis. Disinfectants may be used to clean the wound, which may help in controlling the symptoms of lymphatic filariasis.
The physician may prescribe antibiotics like doxycycline and the patient may have to take antibiotics for a longer period of time to reduce the growth of elephantiasis parasite. However, antibiotics provide only temporary relief. Moreover, these antibiotics cannot be administered to children and pregnant women.
Some drugs such as combination of albendazole and diethylcarbamazine or albendazole and ivermectin may be useful in treating elephantiasis parasite larvae that have not yet reached adulthood. However, it is important to consult a physician before taking any medication in order to ensure that you do not end up worsening your condition.
If antibiotics fail to provide any relief, one may have to resort to surgical procedures to reduce the pain and other symptoms of elephantiasis. Surgery is often conducted in case of genital elephantiasis. In many cases, surgery has to be repeated many times to clear the thick fibrous or fatty tissues and the dead worms. The physician may also advice manual lymph drainage to remove the fluid collected in the affected areas.
Non- filarial elephantiasis may be treated by preventing further infection by keeping the affected areas clean and application of ointment regularly.
If you are living in an area which has high incidence of filariasis, it is advisable to take preventive measures to avoid contracting the disease from an infected person. Ensure that effective controls are taken in your area to prevent breeding of mosquitoes. Wearing shoes while walking and use of mosquito repellent creams and nets may help in preventing elephantiasis from occurring. Talk to your doctor about the feasibility and safety of taking a single preventive dose of diethylcarbamazine if you stay in an area where elephantiasis is highly prevalent. It is very important to keep the parasite or the environmental factors causing elephantiasis at a safe distance in order to save yourself from the trauma and embarrassment caused due to the disease.