Hypovolemic Shock
Last reviewed by Dr. Raj MD on January 12th, 2022.
What is Hypovolemic Shock ?
Hypovolemic shock is a life-threatening condition that happens if you lose more than 20% of your blood supply or fluid supply. Fluid loss will make it impossible for the heart to pump a sufficient amount of blood to the body.
If not treated immediately, it could lead to organ failure and even death. Hypovolemic shock affects both children and adults. The older adults are the most susceptible. (1, 4)
What Causes Hypovolemic Shock?
Hypovolemic shock happens when there is a sudden blood or fluid loss. Causes for hypovolemic shock include the following:
- Excessive bleeding from serious cuts/wounds
- Internal bleeding
- Digestive tract bleeding
- Bleeding from traumatic injuries or accidents
- Profuse vaginal bleeding
- Severe diarrhea
- Burns
- Profuse vomiting
- Excessive perspiration (1, 3, 4)
Image 1 : A cartographic representation of a patient with stab wound who is in high risk for hypovolemic shock.
Photo Source : pinimg.com
Picture 2 : A patient receiving a first aid treatment for hypovolemic shock
Image Source : www.healthcentral.com
Signs and Symptoms of hypovolemic shock
The sings and symptoms vary depending on the severity of the condition. Mild symptoms include the following:
- Cool, clammy skin
- Anxiety
- Agitation
- Confusion
- Decreased to no urine output
- Body malaise
- Pallor (pale skin)
- Headache
- Dizziness
- Rapid breathing
- Light-headedness
Severe symptoms include
- Weak pulse
- Presence of blood in the stool indicating internal bleeding
- Blood in the urine
- Vomiting blood
- Chest tightness
- Swelling of the abdomen
Shock Types Differences : Hypovolemic Vs Anaphylactic Vs Septic Vs Neurogenic
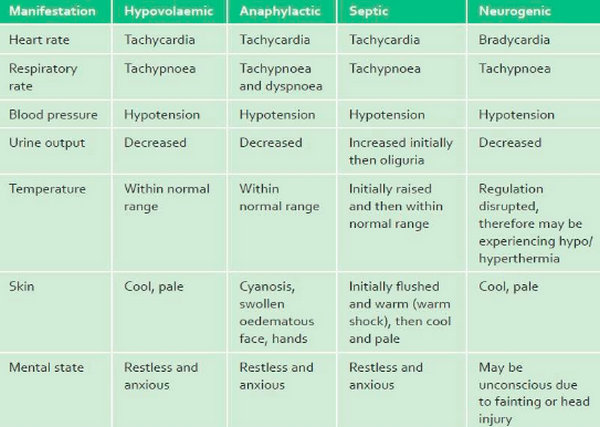
How to deal with Hypovolemic Shock as an emergency situation?
Hypovolemic shock should be dealt with right away for the patient could be dead in just a few hours. If you see someone in hypovolemic shock condition, you have to call for help right away. While waiting for the medical help, you have to make sure that the patient is somehow safe.
Have the patient lie flat and the feet should be elevated for about 12 inches. As much as possible, keep the patient immobilized. Do not give anything by mouth.
You should not elevate the head. If there are dirt or debris in the injury site, then you have to remove it. If there are foreign bodies in the wound such as a knife or a stick, do not remove it to avoid further bleeding. To minimize the blood loss, tie a fabric around the injury site.
What are the possible complications?
- Heart attack
- Gangrene of the arms or legs due to lack of blood supply
- Damage to vital organs of the body like the brain and kidney
- Death
Stages of Hypovolemic Shock
- Stage 1 – The skin of the patient looks pale. The patient demonstrates anxiety and uneasiness. The patient most likely lost 15% of the blood supply, but the breathing and blood pressure are still normal.
- Stage 2 – The patient lost about 30% of blood. Cardinal signs and symptoms include rapid breathing and heart rate. The blood pressure may still be in the normal range but there is a slight deviation in the diastole. The patient feels restless, anxious, and sweating profusely.
- Stage 3 – In this stage, the patient’s blood loss is around 30% to 40%. The systolic reading is less than 100. The heart rate increases rapidly and the breathing is abnormal. The patient is severely agitated, in mental distress, and in anxiety mode. The skin is pale and clammy to touch. The patient is sweating profusely.
- Stage 4 – The blood loss is more than 40%. The pulse is weak and the heart rate increases. It will be extremely difficult for the patient to breathe. The blood pressure drops. The skin is cool, sweaty, and extremely pale. The patient may be in an unconscious state. (4, 5, 6, 7)
How is Hypovolemic Shock diagnosed?
There is no early warning signs for hypovolemic shock. The symptoms will only show once you are in the hypovolemic state. To diagnose the condition, a thorough physical examination should be done. Blood pressure, pulse, and breathing will be checked. Questions will be asked too to assess the responsiveness of the patient.
If there are profuse bleeding, a hypovolemic shock can be easily diagnosed. However, if the patient suffers from internal hemorrhage, it will be quite difficult to predict the presence of hypovolemic shock. Aside from the physical test, the examining physician can also request for blood testing to check if there are electrolyte imbalances. The functions of the liver and kidney will be assessed too.
Other diagnostic testing include the following:
- CT scan/ultrasound of the body organs
- Echocardiogram (ultrasound of the heart)
- Electrocardiogram (assessing the heart rhythm)
- Right heart catheterization (checking the pumping ability of the heart)
- Endoscopy (check the condition of the esophagus and gastrointestinal organs)
- Urinary catheter (check the amount of urine in the bladder) (7, 8)
Hypovolemic shock Treatment
A patient suffering from hypovolemic shock will receive blood products and fluids via the intravenous route. This is to replenish what is lost and to significantly improve the circulation of blood in the body. The damage caused by hypovolemic shock should be stabilized.
Fluids are given to restore what was lost. Medications are given to strengthen and improve the condition of the heart and other vital organs in the body. As per the order of the attending physician, the following fluids and medications should be given: the
- Intravenous crystalloids
- Platelet transfusion
- Blood plasma transfusion
- Red blood cell transfusion
- Dopamine
- Epinephrine
- Dobutamine
- Norepinephrine
- Antibiotics to prevent infection and septic shock (5)
Hypovolemic Shock in children
In children, hypovolemic shock is the leading cause of morbidity and mortality. To diagnose the condition, the child should be subjected to a thorough physical examination, vital signs monitoring, and gathering of important laboratory data. Severe dehydration, injury, and blood disorders are the leading causes of hypovolemic shock in children.
Hypovolemic Shock in older adults
Hypovolemic shock is very dangerous in older adults. They have a higher mortality rate than the younger ones. Older adults have less tolerance for shock. Hence, older patients should be treated right away to prevent further complications.
Recovery Time
The recovery of the patient suffering from hypovolemic shock depends on the patient’s age, degree of shock, and medical condition. Patient with mild degree of shock tend to recover more easily than those with severe shock. Patients with severe organ damage may take some time to fully recover.
A course of extensive medications should be given to help the patient recover from the shock. In fact, there are instances wherein the organ damage is irreversible. Severe hypovolemic shock could lead to death, especially in the case of older adults.
Resources :
- www.healthline.com
- https://en.wikipedia.org
- emedicine.medscape.com
- http://www.medicalnewstoday.com
- www.ehealthstar.com
- wps.prenhall.com
- www.howshealth.com
- The Washington Manual of Critical Care edited by Marin H. Kollef, Timothy J. Bedient, Warren Isakow