Dry Sockets
Last reviewed by Dr. Raj MD on January 12th, 2022.
In this article, you will find the information you need to better understand dry socket. It begins with a clear definition of a dry socket as well as a brief description of needed anatomy.
Next, this article covers a general description, causes, symptoms, treatments and of course preventative measures. This article will be informative and medically based, although, there are home remedies added.
Anatomy
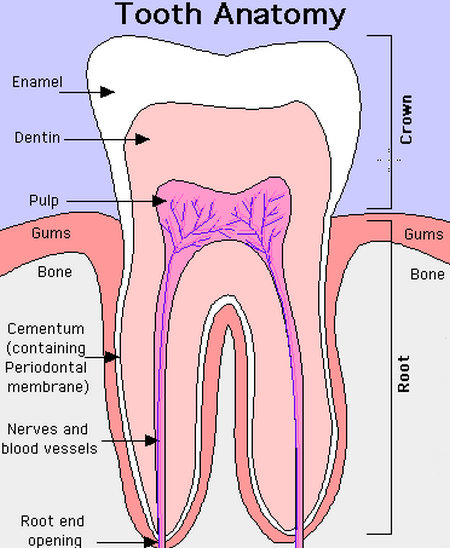
Image 1: The gums create the blood clot that would cover and protect the bone.
Picture Source : www.enchantedlearning.com
A socket is nothing more than the area left from an extracted tooth where the roots of the tooth once where. The jaw is completely made up of bone tissue as well as the tooth sockets with a small amount of skin tissue or gums as a covering.
The teeth are connected directly to the bone of the jaw and are held in place by a thin ligament. Although thin they are very strong which is why your teeth do not fall out even when eating sticky or hard things. (1,9)
What is dry socket ?
The medical name for a dry socket is Alveolar osteitis which in short means that the bone under a removed tooth is inflamed. When a tooth is removed a blood clot forms which protects the alveolar bone. If this clot is dislodged then the bone is exposed and susceptible to this inflammation. This usually occurs 3-4 days after the removal of the tooth. (7,16)
There has been a great discussion about the terminology surrounding “dry sockets.” The term dry socket was first used in medical writing in 1896 but since then medical writers have used other terms. Alveolar osteitis is the most common but other names have been used, such as alveolitis, alveolitis sicca Dolorosa, alveolar osteitis, localized alveolar osteitis, septic socket, fibrinolytic alveolitis, necrotic socket and alveolar just to name a few.
The best definition of dry sockets is postoperative pain which is around the tooth extraction site. This pain increases in those first few days after the operation. (6,8,9)
Here are a few key points about Dry Sockets
- It is painful
- Only happens after Permanent tooth extraction and clot movement or malformation.
- The pain is due to bone exposure and therefore inflammation.
- Usually, initiates a few days after tooth extraction.
- Strong pain medications are needed (6,8,9,10)
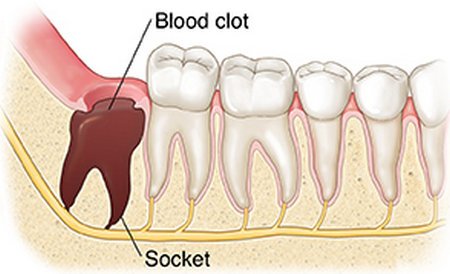
Figure 2: The blood clot fills the socket and protects the bone as well as the nerve.
Photo Source : www.fairview.org
What is a Dry Socket with wisdom teeth?
Most people hear of dry sockets related to wisdom teeth. This is because it is the most common reason for tooth extraction. But in reality, dry sockets can happen with any type of tooth extraction.
What causes Dry Sockets?
The following things could increase the chance of getting dry sockets.
Risk factors include:
- A difficult surgery or trauma during surgery
- Lack of experience from medical personnel involved.
- Wisdom tooth or Mandibular Third Molar extraction.
- Another diagnosis including systemic disease
- Taking oral contraceptives
- Studies have shown that gender can play a role in the chances
- Smokers
- Dissolved or moved clots
- Infection
- Cleaning too much or aggravating the surgical area.
- Patients age
- Extraction of multiple teeth
- Anesthetic use which may cause vasoconstriction.
- Remaining bone or root fragments
- Closure used such as sutures or flap design. (6,8,9,11,14)
The following are common causes:
- Smoking
- Drinking from a straw,
- Periodontal disease
- Hormone replacement therapy.
- Bacterial infection
- Trauma to the surgical area
- Lack of care for the surgical area (6,8,9,10,11,12,13,14)
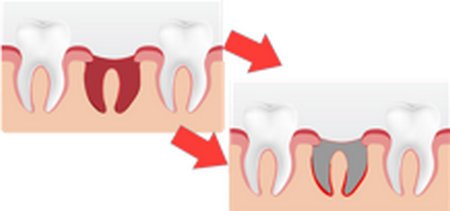
Figure 3 : How the socket looks when the blood clot is dislodged.
Photo Source : www.joseylanedentistry.com
Why does smoking or drinking from straws cause Dry Sockets?
As you smoke or drink from a straw you do a sucking motion with your cheeks. This motion also causes suction on the surgical site. This can cause the clot which is protecting the bone to be dislodged and therefore cause inflammation and pain.
Will getting Dry Sockets cause other complications?
Usually, there are no complications to having a dry socket other than pain. Rarely infection is noted and only in grave cases. It could, however, incite slower healing processes. (6)
Dry socket Symptoms
- The most prominent symptom is severe pain.
a. The pain could radiate, usually to the ear and temporal region.
b. At times there could be pain in the jaw and orbital or eye regions. - Bad breath
- Low fever
- Inflamed and swollen gums
- Grayish discharge in severe cases
- Complete or total loss of blood clot which looks just like an empty hole
- Visible bone
- Bad taste (6,8,12,13,14,16)
When do I need to go see a doctor?
- Pain worse than what your doctor told you to expect.
- Pain uncontrolled by Tylenol. (6)
What does a Dry Socket look like : Pictures
The exam is basically unremarkable. A doctor will be able to notice that the blood clot is not in its place. Other than that there is no other noticeable sign (16)
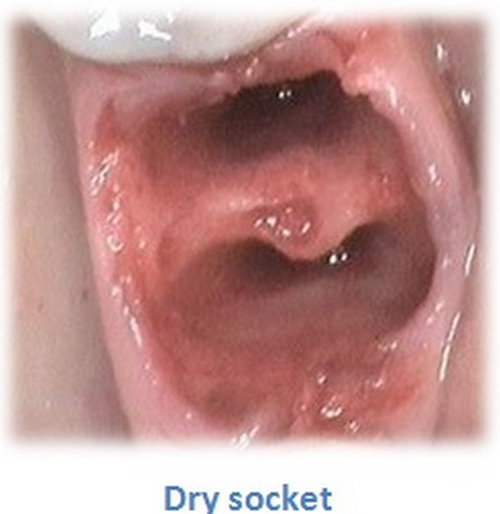
Figure 5 : In this image you can clearly see that the hole is completely empty. This means that the blood clot that should be filling the space has been dislodged and the bone is exposed.
Image Source : www.identalhub.com
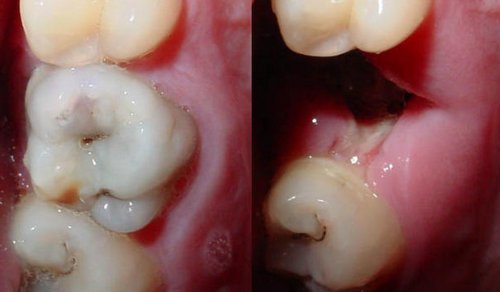
Photo 6 : The socket where the tooth once was. It is hard to tell if there is still some blood clot left inside.
Picture Source : www.identalhub.com
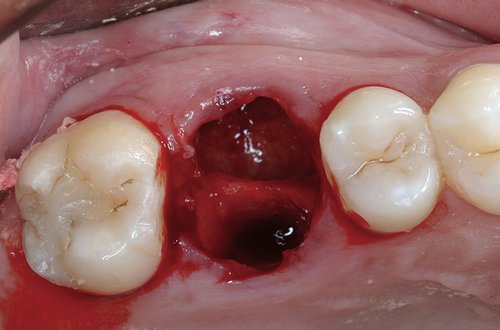
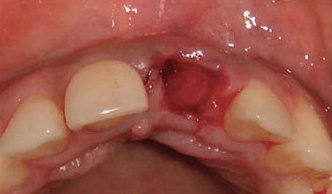
Image 8 : From this angle it is hard to tell if the patient indeed has a dry socket. This is why it is important to be checked by a dentist.
Figure Source : www.jaypeejournals.com
Dry socket Treatment
- Pain management until the healing process is complete.
a. Systemic analgesics (not nonsteroidal anti-inflammatory drugs or narcotics)
b. Dental block
c. Intra-alveolar packing. Packing the wound with analgesics. - Remove partially dissolved clot or debris by cleaning the area using lavage or suction.
- Good personal hygiene
- Antibiotics in the case of infection.
- X-rays to be sure there are not bone or root fragments (6,8,12,13,14,15,16)

Image 4: The types of syringe used to clean out the socket as well as apply the dry socket gel.
Picture Source : dentistrydonedifferently.files.wordpress.com
How to Prevent Dry Socket
- Antibiotics before surgery
a. Topical or systemic - Lavage using Chlorhexidine
- Lavage using Para-Hydroxybenzoic Acid
- Lavage using Tranexamic Acid
- Lavage using Polylactic Acid
- Administration of steroids to avoid inflammation.
- Packing with a dressing impregnated with Eugenol
- Extensive lavage during surgery
- Use of 9-aminoacrinide (antiseptic)
- Sterile procedure (3,4,5,14,16)
What is Dry Socket paste?
This is a material which helps take the place of the dislodged or dissolving the blood clot and also gives pain relief. Cross-linked dextran plymer (Debrisan), available in bead or paste form. Usually will only need two treatments.
Its specific indications for use are as follows:
- Do not use if you are sensitive to guaicol or eugenol
- Do not use if you are pregnant without doctor consent.
- Should be placed by a dentist.
- Do not ingest the packing
- Used when socket does not have the clot and possibly is full of debris.
- Socket should be cleaned before placement
- Place the gel or bullet with a syringe and tap lightly to be sure all bones is covered
- Dry socket paste and bullets do not need covering
- Will slowly wash out as the socket heals, removal is not necessary.(2,15)
Dry Socket Home remedies
Your dentist or doctor should be aware of any home remedies that you plan to use. Even the sites noted in this article express that the best treatment for dry sockets is with your doctor.
The remedies listed below are to help you until you are able to be seen by your doctor.
Most home remedy sites agree that the best treatments for dry sockets are as follows:
Use of clove oil packing
It is the same ingredient in the dry socket gel (eugenol)
- Made using a small piece of gauze impregnated with the clove oil and placed into the tooth socket. This dressing should be removed within 24 hours.
- This treatment could cause worse issues including tissue damage and bone death. This should only be used as a first aid until a doctor is available to examine and treat the dry socket.
Honey
- Made using a small piece of gauze impregnated with honey.
- This is basically trying to replicate the blood clot and should only be used for 24-hour sand in emergency situations
- Does not have a pain relief effect but does decrease inflammation, therefore, lowering pain levels.
How long does it take for a Dry Socket to heal?
The pain from a dry socket will be gone within a day or two of treatment initiation. Treatment can last up to a week or a week and a half depending on the healing factors of each individual. These factors include good oral hygiene, if the patient smokes, and proper diet.
In conclusion dry sockets happen after tooth removal when the blood clot is dislodged or starts to degenerate. This has various causes and should be avoided.
When a dry socket happens it causes much pain. Targeting this pain is the main course of treatment until proper healing can occur.
References:
- https://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0025304/
- https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=3ac8133e-e5ac-42f1-9ce6-80eee07b83bb
- https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0050315/ What treatments can be used to prevent and treat alveolar osteitis (dry socket)? This version published: 2012; Review content assessed as up-to-date: November 07, 2012.
- https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0025231/ Effect estimates and methodological quality of randomized controlled trials about prevention of alveolar osteitis following tooth extraction: a systematic review L Hedstrom and P Sjogren.
- https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0022003/ Prevention of alveolar osteitis with chlorhexidine: a meta-analytic review A Caso, LK Hung, and OR Beirne
- https://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0023282/
- http://www.mayoclinic.org/es-es/diseases-conditions/dry-socket/home/ovc-20305925
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2905714/ Alveolar Osteitis: A Comprehensive Review of Concepts and Controversies Antonia Kolokythas,* Eliza Olech, and Michael Miloro
- http://www.jcda.ca/article/d54
- http://www.lenus.ie/hse/bitstream/10147/236012/1/DecJanart2.pdf The management of dry socket/ alveolar osteitis
- https://www.researchgate.net/publication/273250883_Dry_Socket_Alveolar_Osteitis_Incidence_Pathogenesis_Prevention_and_Management
- Oral and Maxillofacial Surgery edited by Lars Andersson, Karl-Erik Kahnberg, M. Anthony Pogrel https://books.google.com.mx/books?id=7tuUooCL47oC&pg=PA564&dq=Alveolar+Osteitis&hl=en&sa=X&redir_esc=y#v=onepage&q=Alveolar%20Osteitis&f=false
- Cawson’s Essentials of Oral Pathology and Oral Medicine By Roderick A. Cawson, Edward W Odell https://books.google.com.mx/books?id=K035mlSXAAsC&pg=PA104&dq=Alveolar+Osteitis&hl=en&sa=X&redir_esc=y#v=onepage&q=Alveolar%20Osteitis&f=false
- Shafer’s Textbook of Oral Pathology By Arya Rajendran, B SivapathasundharaM https://books.google.com.mx/books?id=WnhtAwAAQBAJ&pg=PA603&dq=DRY+SOCKETS&hl=en&sa=X&redir_esc=y#v=onepage&q=DRY%20SOCKETS&f=false
- The Removal of Teeth with Forceps By Robin W Matthews, Christopher N Bell https://books.google.com.mx/books?id=a5YlhjJqcxsC&pg=PA29&dq=DRY+SOCKETS&hl=en&sa=X&redir_esc=y#v=onepage&q=DRY%20SOCKETS&f=false
- Emergency Medicine: Expert Consult – Online By James G. Adams https://books.google.com.mx/books?id=Q2Ag9OKC7awC&pg=PT814&dq=DRY+SOCKETS&hl=en&sa=X&redir_esc=y#v=onepage&q=DRY%20SOCKETS&f=false
- https://www.animated-teeth.com/dry-sockets/a-dry-socket-home-remedy.htm
- https://authorityremedies.com/home-remedies-for-dry-socket/