Melena
Last reviewed by Dr. Raj MD on January 12th, 2022.
Melena Definition
The usual color of the stool is light brown to dark brown and it is linked with the decomposition of food and presence of bilirubin.
For some reasons, the stool’s color is altered. Black coal tar colored stool is medically called melena stool. It is caused by bleeding in the upper gastrointestinal track, specifically in the stomach and duodenum. In rare instances, the bleeding originates from the mouth or nasal cavity. (1)
Why is Melena black?
Why is the color of the stool black coal tar? It is linked with the decomposition of iron from haemoglobin. As blood passes down from the gut to the rectum, air, bacteria, and digestive enzymes take their action. It leads to the breakdown of blood cells and changes the color of the stool from dark maroon to black. (1, 2)
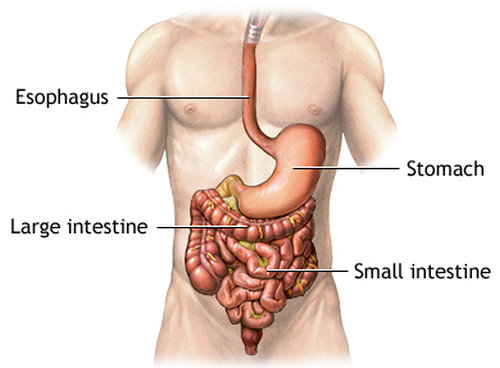
Image 1 : An anatomical presentation of the gastrointestinal tract.
Picture Source : keckmedicine.adam.com
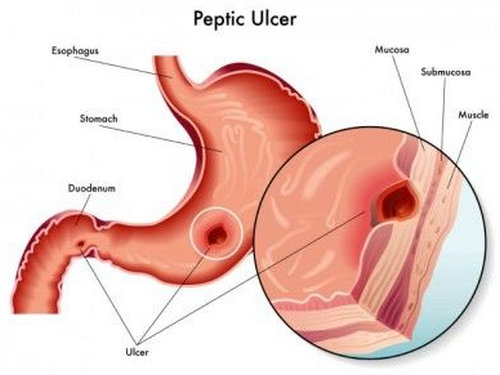 Photo 2 : Peptic ulcer, one of the common reasons for GI bleeding leading to melena
Photo 2 : Peptic ulcer, one of the common reasons for GI bleeding leading to melena
Image Source : s-media-cache-ak0.pinimg.com
Melena vs hematochezia
Hematochezia pertains to bloody stools. The blood in the stool appears fresh and bright red to maroon in color. It is indicative of bleeding in the lower gastrointestinal track, specifically in the large intestine, rectum, and anus. Hematochezia can only be noticed once you wipe the anus or when the red strands stain the toilet bowl. (2)
Melena associated symptoms
- Black tarry stool (2, 3)
- Coffee ground material in the vomitus
- Pale skin
- Lightheadedness
- The patient feels tired easily
- The abdomen is distended
- Shortness of breath
- Low blood pressure (hypotension) (3)
- Rapid heart rate (tachycardia)
- Abdominal pain
Melena Causes
- False melena – The discoloration of the stool is not caused by blood. It is usually caused by taking colored foods such as black licorice, blueberries, and too much intake of chocolate. Other contributing factors include too much iron, especially in patients taking iron supplement, lead intake, and side effects of medications like pepto-bismol. (3, 4)
- Internal bleeding – Melena is usually a result of upper gastrointestinal bleeding. The causes of bleeding include the following:
- Bleeding ulcer – Peptic ulcer causes sore or open wound in the duodenum or stomach. The primary reason for peptic ulcer is H. pylori bacteria infection. The bleeding can also be caused by prolonged use of non-steroidal anti-inflammatory drug like aspirin. Such drugs affect the protective coating of the lining of the stomach.
- Esophageal varices – The veins in the esophagus dilate secondary to high blood pressure in the hepatic circulation. It can also be due to liver cirrhosis. Ruptured varices cause profuse bleeding in the upper GI tract, which leads to the discoloration of the stool.
- Gastritis – It is the inflammation of the gastric mucosa, which is caused by excessive consumption of alcoholic beverages and heavy smoking. Other forms of diseases can cause gastritis such as pernicious anemia and bile reflux. An inflamed stomach increases the possibility of bleeding. (3, 4,5)
- Mallory-Weiss tear- It pertains to the tear in the lower esophagus and is associated with persistent coughing, violent vomiting, and convulsions.
- Hemorrhagic fever – It is caused by a virus-carrying mosquito, which attacks the platelets. Platelet plays a very important role in clotting the blood. Not having enough platelet could make a patient susceptible to bleeding, not only in the GI tract, but as well in various parts of the body. (6)
Which test would tell the presence of melena?
To correctly diagnose melena, various medical procedures should be performed. The doctor will conduct a thorough medical history, which will assess the patient’s dietary habit and medication intake, especially prolonged used of non-steroidal anti-inflammatory drugs. Test performed to identify the presence of melena includes the following:
- Fecal occult blood test – This is done to check the presence of red blood cells in the stool. A fresh stool sample is collected and check under the microscope.
- Barium studies/Upper GI series – The patient should ingest a barium solution to take an x-ray of the upper gastrointestinal tract. This test is done to thoroughly examine the GI tract for any presence of ulceration or obstruction.
- Esophagogastroduodenoscopy (EGD) – A small camera is passed through the patient’s mouth to visualize the upper GI tract, particularly the stomach, esophagus, and duodenum. Through this test, any ulceration or varicosities will be thoroughly checked.
- Blood test – This is to detect the effect of bleeding in the body. Blood components are checked, especially the red blood cells, haematocrit, and haemoglobin. (5, 6, 7,8)
How to cure/treat melena?
What is the best melena treatment? Melena is not a disease itself. It is an indicator that something is not right in your body. To cure melena, you need to find out the underlying cause. To control the bleeding and reduce the damage to the body, the patient should receive intravenous fluids and blood transfusion, especially if a lot of blood is lost.
The patient is also put on proton pump inhibitor. Upper and lower gastrointestinal tract endoscopy can help control the bleeding. In severe cases, a surgery is performed.
If the bleeding is caused by esophageal varices, a catheter balloon should be inserted to stop the bleeding. To constrict the blood vessel, gastric washing is done using cold saline solution. This can help stop the bleeding.
If the bleeding is not stopped, the patient could suffer from hypovolemic shock. It is a life-threatening condition. If you notice blood in your stool along with other associated symptoms, you should immediately consult your doctor for proper diagnosis and treatment. (8, 9,10)
What you can do to prevent melena?
Melena can be prevented by avoiding the things that could lead to bleeding of the upper GI tract. Simple measures to prevent melena include the following:
- Use non-steroidal anti-inflammatory drugs with high caution. If you are going to take NSAIDs, make sure you take it on a full stomach to prevent gastric upset.
- Reduce your consumption of alcoholic beverages. Too much intake of alcoholic drinks could lead to irritation of the esophagus and stomach.
- Smoking can adversely affect the lining of the stomach. It is highly recommended to quit smoking.
- Increase your intake of fiber rich foods like green leafy vegetables and fruits.
- Limit your exposure to stress to prevent excessive production of hydrochloric acid.
- Make it a habit to eat three full meals a day. Do not skip meal as empty stomach gets irritated easily. (5, 6,7)
References:
- http://healthsurgical.com
- http://www.tandurust.com
- https://en.wikipedia.org
- www.healthhype.com
- www.wisegeekhealth.com
- ic.steadyhealth.com
- wakegastro.com
- www.medicinenet.com
- www.medicinenet.com
- https://medlineplus.gov